Knee pain can be caused by disease (arthritis) or injury (direct trauma, repeated stress, or sudden movement that is beyond the knee’s normal range ). Knee pain can also be caused by incorrect positioning of the kneecap, weakness of muscles that control the hip and knee, flat feet, muscle imbalances in the back and pelvis, and tightness of the ITB (iliotibial band) or other muscle groups that cross the knee. This can limit range of motion in the knee, decrease muscle control in the affected leg and reduce the strength and endurance of the muscles around the knee (and hip. A person’s ability to get up from a chair, walk long distances, climb stairs, or play sports is ultimately affected due to pain in the knee. Physical therapists are trained to evaluate the cause of knee pain and develop treatment plans to return individuals to their prior level of function.
ANTAOMY
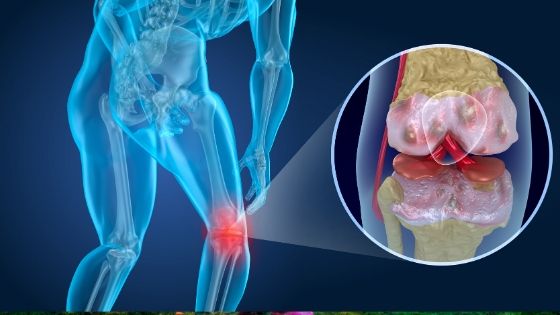
The knee joint consists of the articulation of the femur (upper leg bone), with the tibia (shin bone) and the patella (knee cap). There are several ligaments that provide stability to the knee joint including the anterior cruciate ligament (ACL), posterior cruciate ligament (PCL), medial collateral ligament (MCL) and lateral collateral ligament. There are multiple muscles and supporting structures surrounding the knee including the quadriceps, hamstring, and gastroc (calf muscle) and ITB band.
DIAGNOSIS
Your physical therapist can diagnosis your problem based on your symptoms, medical history, and a thorough examination. The therapist will look for:
- Pain or tenderness in the knee
- Instability or “giving way” in the knee
- Decrease in motion of the knee, hip, back, and/or ankle
- Decrease in strength of muscles surrounding the knee as well as core and hip muscles
- Pain, weakness, or dysfunction with going up and down stairs
- Difficulty walking or abnormal walking pattern
- Difficulty getting out of a chair
- Problems with balance
- Difficulty performing sport specific activities
TREATMENT

- Manual therapy (hands on techniques)
- Mobilizing the joints to improve motion and decrease knee pain
- Soft tissue techniques to increase blood flow to improve motion and decrease pain
- Stretching to improve flexibility
- Exercise
- Functional exercises designed to return you to your home, work, and/or sport specific activities (for example, sit to stand, stairs, etc) including balance and stability exercises
- Specific therapeutic exercises to work on strength, flexibility, endurance and range of motion to address your specific goals
- Patient education
- Diagnosis/anatomy
- Self-management of pain
- Home exercise program
- Postural education
- Use of modalities (heat, ice)
CORTICOSTEROIDS FOR KNEE PAIN
A recent clinical trial demonstrated physical therapy was superior to steroid injections in decreasing pain and disability. Corticosteroid injections have been shown to have potential harmful effects on joint cartilage, especially at higher doses. Evidence also supports the possibility of accelerated OA or rapid OA progressions (which is the rapid loss of joint space on x-ray ) after injection that is at a rate faster than expected. These individuals will likely need joint replacements earlier than expected.
Our physical therapists at Lifeline Therapy take the time to individualize a treatment plan for you for the best possible outcomes. We work one-on-one with our patients, utilizing hands-on, evidence based manual techniques and treatments that yield successful and functionally meaningful outcomes. Physical therapists are the movement experts and can be your first point of contact if you start to feel pain in your knee. Don’t let knee pain prevent you from living your fullest life! Contact us today!
References:
Kompel, A. J., Roemer, F. W., Murakami, A. M., Diaz, L. E., Crema, M. D., & Guermazi, A. (2019, December). Intra-articular Corticosteroid Injections in the Hip and Knee: Pherhaps Not as Safe as We Thought? Radiology, 293(3), 656-663. doi:https://doi.org/10.1148.radiol.2019100341
Guideline for the management of knee and hip osteoarthritis, second edition. Royal Australian College of General Practitioners. July 2018.
Gail Deyle, D.Sc., professor, Brooke Army Medical Center, San Antonio, Texas; Etan Sugarman, M.D., orthopedic surgeon, Lenox Hill Hospital in New York City; New England Journal of Medicine, April 8, 2020