By Dr. Shelby Hoblit, PT, DPT
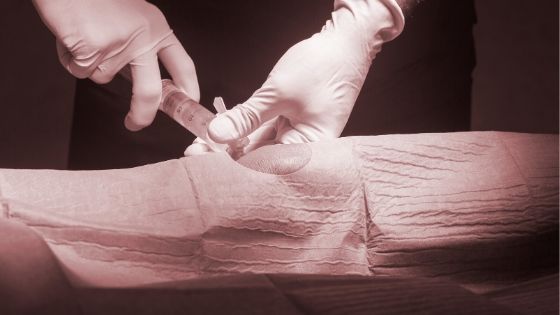
People considering receiving corticosteroid (ex: Cortisone) injection to address pain caused by hip or knee osteoarthritis (arthritis) may want to consider recently published facts with regard to effectiveness of the injections, and possible consequences.
Osteoarthritis (OA) is the most common type of arthritis, is a normal age-related change, and is characterized by the wearing down of the protective cartilage that cushions the ends of your bones. These changes are evident upon x-ray imaging. The American College of Rheumatology generally recommends corticosteroid injection to be considered for those individuals with moderate to severe pain, in which the pain has not responded to anti-inflammatory oral medications like Advil or Ibuprofen. However, the American Academy of Orthopedic Surgeons does not currently have recommendations for or against the use of corticosteroid injection. They suggest that physician providers should be aware of new and emerging evidence to determine if the possible benefits outweigh the possible risks. According to literature reviews of studies completed on patients receiving these injections into either hip or knee, overall quality of evidence was graded as low due to inconsistency in the effects of injections on pain and function. Additionally, studies have shown that individuals with more progressed disease changes in the joint like meniscal damage, or greater joint space narrowing are less likely to respond favorably to injections in the long term.
Corticosteroid injections: evidence with regard to joint damage
Evidence supports that these injections can have harmful effect on joint cartilage especially at higher doses. When compared with placebo or non-treatment injection, corticosteroid injection in the knee resulted in greater cartilage volume loss and provided no significant difference in knee pain 2 years after injection. These findings were confirmed in another study which showed individuals who received corticosteroid injection in the knee had worsening osteoarthritis symptoms evident on x-ray compared to those who did not receive the injection. With regard to cortisone injections for the hip, similar evidence has been supported in patient studies.
Potential adverse joint events: know the risks!
When having a procedure like this done, it is important for individuals to be aware and know that they are at risk for potential harmful or adverse events. Although these events aren’t commonly observed, it is important to be informed. With regard to corticosteroid injection, evidence supports the following possible events after injection:
- Accelerated OA or rapid OA progressions which is the rapid loss of joint space on x-ray that is at a rate faster than expected.
- These individuals will likely need joint replacement earlier than expected.
- Subchondral insufficiency fracture (type of stress fracture which occurs below the cartilage on the weight bearing surface of a bone) of the knee and hip.
- These patients present with acute pain following injection which gradually worsens for a week with no known mechanism or trauma. When diagnosed early, can heal fully. Delayed diagnosis can lead to collapse of the joint surface.
- Complications with osteonecrosis (the death of bone tissue due to a lack of blood supply).
- This disease mostly affects the hip bone, requiring MRI to diagnose. Patients present with insidious onset of pain, and likely require treatment for fracture of joint surface collapse.
- Rapid joint destruction including bone loss.
- This process may be related to the aforementioned subchondral insufficiency fracture or necrosis.
It is important to note that some patients who develop rapid joint space loss tend to have no or mild arthritic changes on x-ray screen initially. Despite the frequency of which these injections are performed, large studies looking at past patients and studies that follow patients after injection are lacking.
What does the current evidence recommend?
The American Physical Therapy Association has analyzed available data and compiled recommendations of strongest, moderate, and low levels of evidence with regard to treatment options for knee and hip OA. The evidence suggests treatment emphasis on self-management and non-surgical options.
- Strongest evidence:
- Land-based exercises to improve function. These are individualized, progressive restive exercises for strengthening specific muscle groups to help support the joint. Your physical therapist is equipped with special training to evaluate your symptoms, and design a program tailored to fit your needs. Your physical therapist will monitor your progress, and teach you how to manage your symptoms at home long-term.
- Weight management. Evidence supports achieving and maintaining a healthy body weight to help manage condition and symptoms.
- Moderate evidence:
- Oral non-steroidal anti-inflammatory medications such as Advil or Ibuprofen to manage symptoms.
- Very low evidence:
- Corticosteroid injections for hip or knee.
As we age as a population, it is likely that more and more individuals will be affected by osteoarthritis. It is important to understand treatment options, risks of certain treatments, and what are the best recommendations for treatment going forward.
Sources:
Kompel, A. J., Roemer, F. W., Murakami, A. M., Diaz, L. E., Crema, M. D., & Guermazi, A. (2019, December). Intra-articular Corticosteroid Injections in the Hip and Knee: Pherhaps Not as Safe as We Thought? Radiology, 293(3), 656-663. doi:https://doi.org/10.1148.radiol.2019100341
Guideline for the management of knee and hip osteoarthritis, second edition. Royal Australian College of General Practitioners. July 2018.
Gail Deyle, D.Sc., professor, Brooke Army Medical Center, San Antonio, Texas; Etan Sugarman, M.D., orthopedic surgeon, Lenox Hill Hospital in New York City; New England Journal of Medicine, April 8, 2020